Parkinson’s Disease and the Gut Microbiome
What are we learning about this debilitating condition and the relationship with your gut ?
GUT SKIN CLINIC Neutral Bay Sydney
I am on a mission to educate and empower you, supporting you to stay healthy using clear science and best practices.
This blog does not replace a practitioner consultation nor is it to be seen as personalised advice.
In this last year, I am welcoming more patients with Parkinson’s disease (PD) into clinic.
High profile sufferers have raised awareness internationally.
Michael J Fox
Billy Connoly
Alan Alda
Ozzy Osbourne
Robin Williams
Linda Rondstat
According to global data published in The Lancet, Neurology, the number of people living with Parkinson’s disease more than doubled between 1990 and 2016, making it the fastest-growing neurological disorder worldwide (Dorsey et al., 2018; GBD 2016 Neurology Collaborators, 2019).
I have reviewed some of the most impactful and highly cited reserach papers and created this summary for
Patients diagnosed with Parkinson’s disease
Anyone with a strong family history of PD
Anyone experiencing chronic constipation
Everyone seeking prevention-focused care in Sydney
Individuals wanting microbiome testing Australia wide.
For patients in Sydney seeking a functional perspective, this evolving research shifts the conversation from simply managing symptoms to understanding upstream drivers.
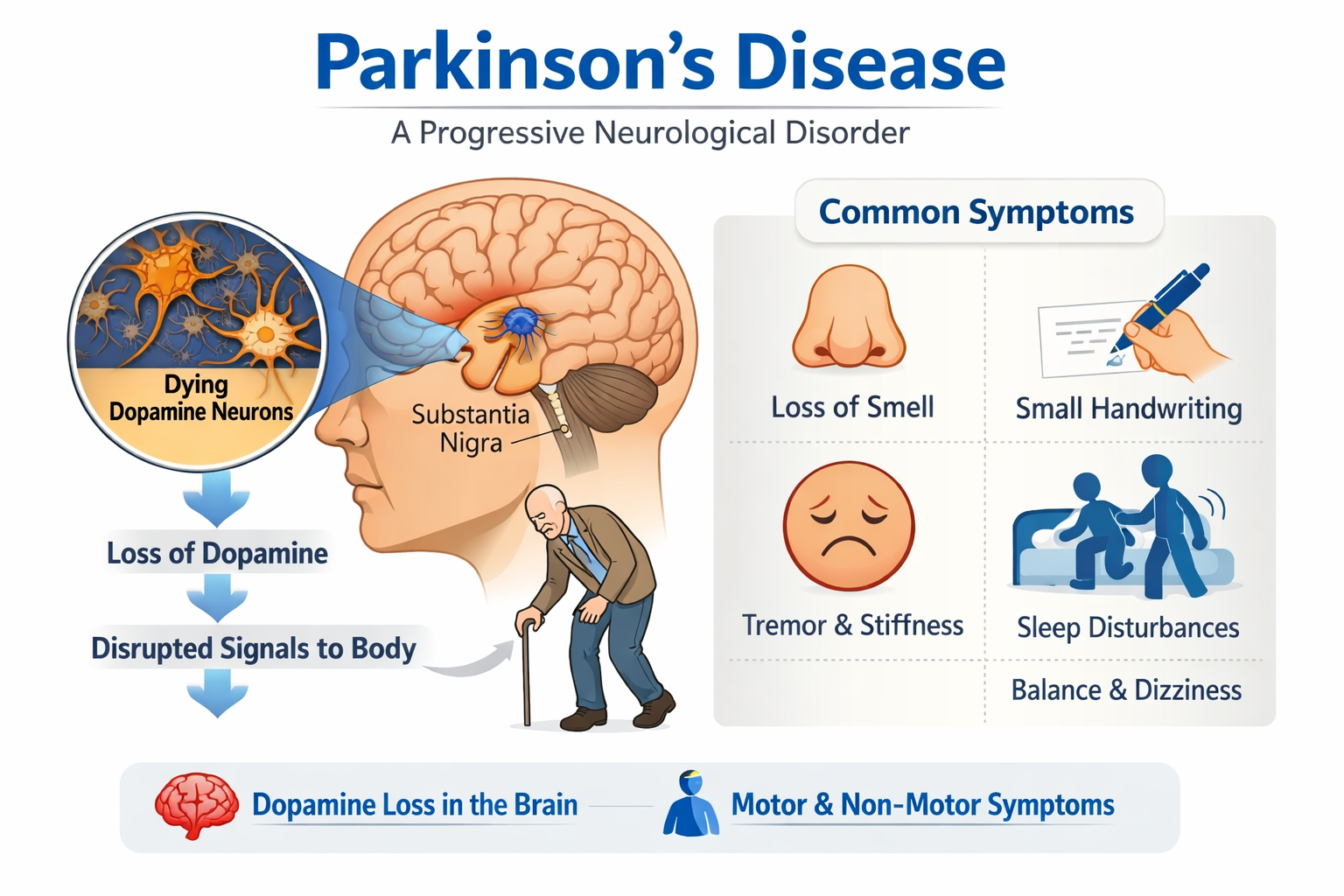
Parkinson’s disease is a progressive neurological condition caused by the gradual loss of dopamine-producing nerve cells in the brain. Dopamine is a chemical messenger that helps regulate movement, mood and many automatic body functions.
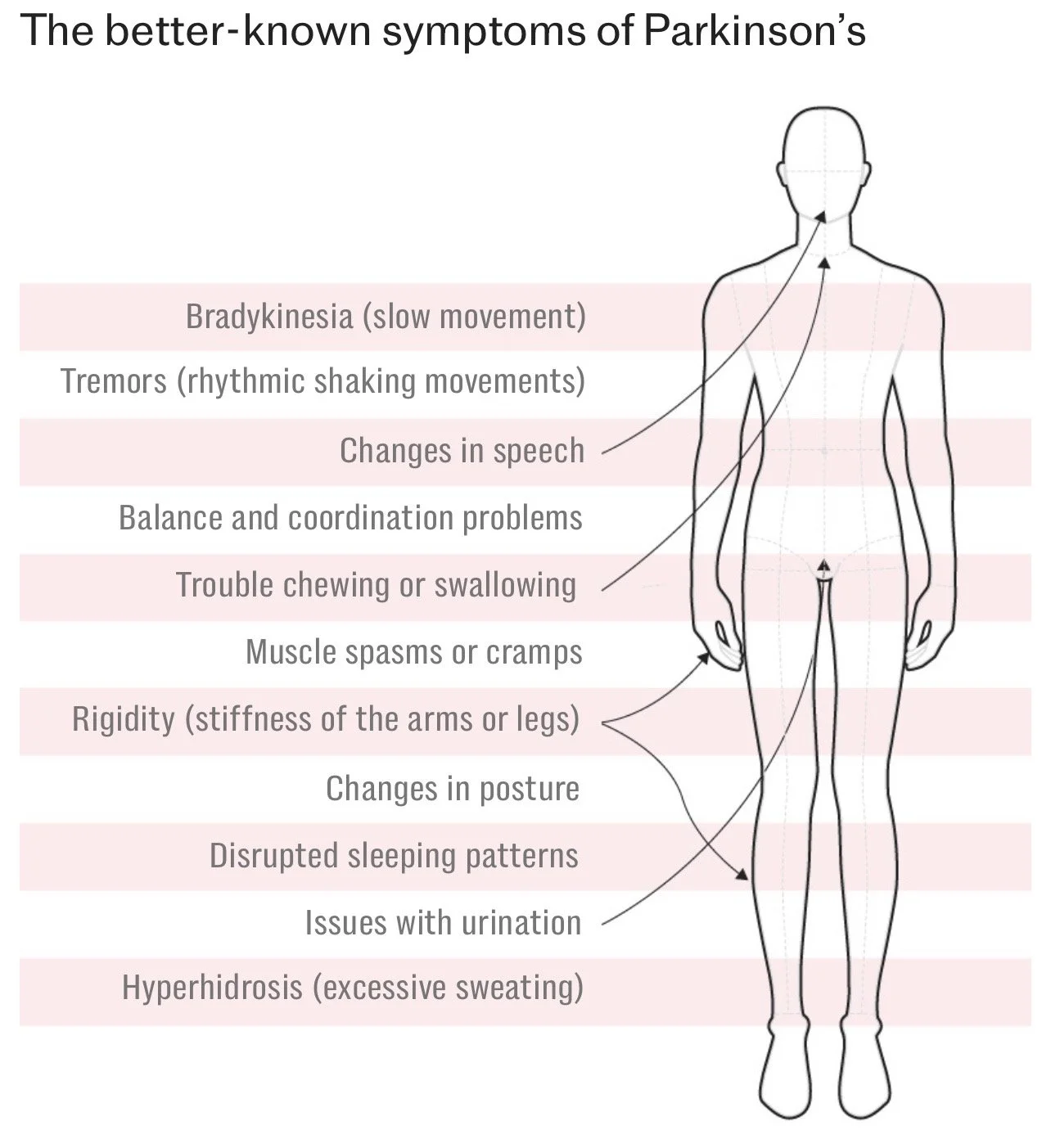
Although tremor is the symptom most people associate with Parkinson’s,
many early changes can appear years—sometimes decades—before diagnosis, and many are not related to movement.
Recognising these early signals may allow earlier assessment and management.
While ageing contributes to PD risk, it does not fully explain the rise and there are likely multiple proposed mechanisms implicated.
Increasingly, research is exploring
Environmental exposures
Metabolic health,
Inflammation — and my passion, the Gut microbiome.
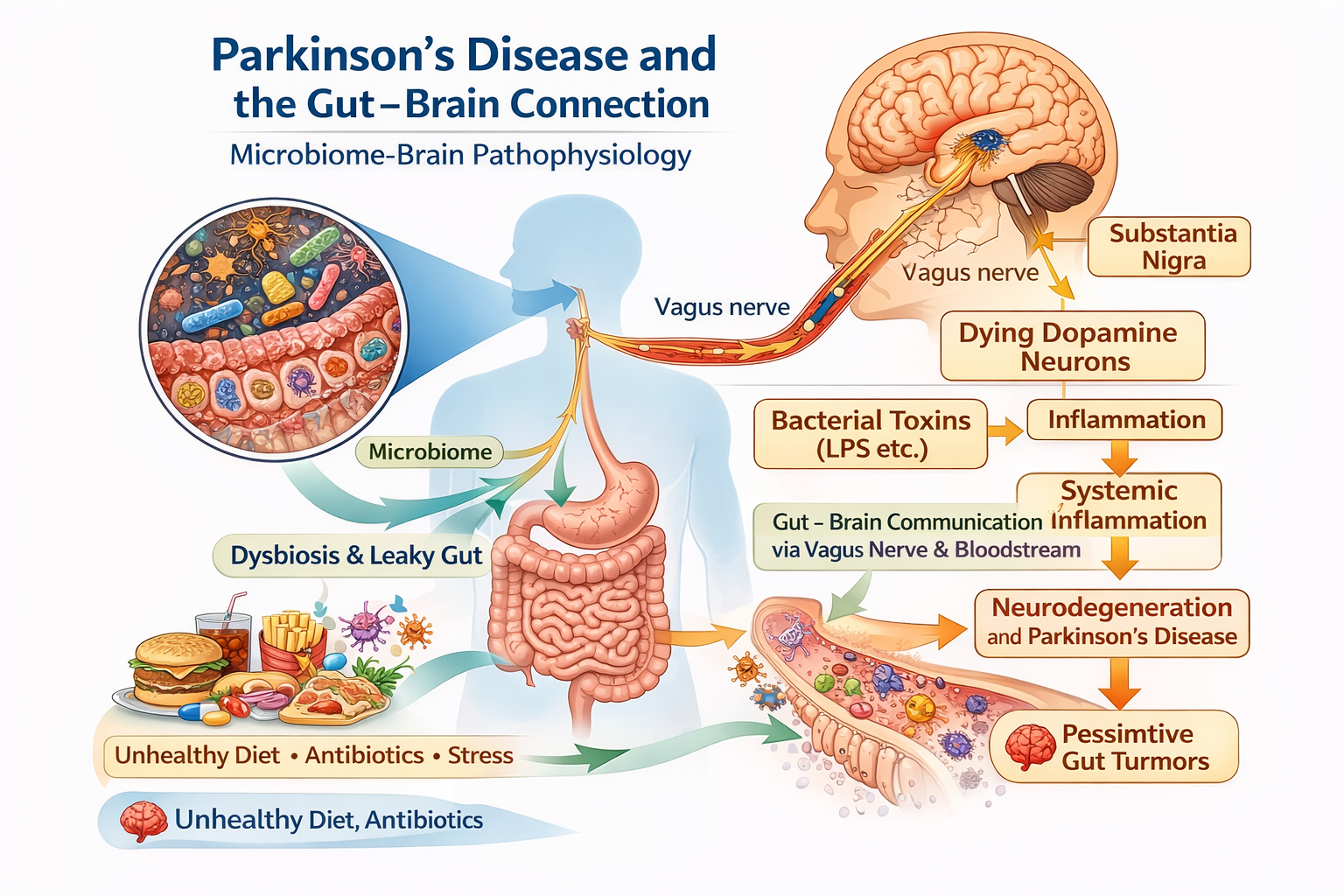
Gut Brain Axis and Parkinson’s Disease
Interestingly, many individuals diagnosed with Parkinson’s disease report years of digestive symptoms — particularly constipation before motor symptoms appear.
Neuropathologist Heiko Braak proposed that Parkinson’s pathology may begin in the gut before travelling to the brain via the vagus nerve.
In the last 5 years, this “gut-first” hypothesis has gained increasing scientific support.
Key Research Linking the Microbiome & Parkinson’s
Large-Scale Human Microbiome Data
A 2022 study by Zachary D. Wallen published in Nature Communications examined hundreds of individuals with Parkinson’s disease.
Findings included:
Significant alterations in microbial species with over 30% of microbial species and metabolic pathways testing significantly differenet between PD sufferes and controls.
Changes in inflammatory and immune signalling pathways
Reduced butyrate-producing bacteria (important for gut lining integrity and production of anti inflammatory supports)
This is suggestive that functional disruption in the gut may play a role in PD progression.
Mechanistic Reviews
A comprehensive review in Brain Research (Nielsen et al., 2021) showed:
Consistent microbiome changes across global PD cohorts, occuring BEFORE clinical motor symotoms.
Animal testing models required certain microbiota to develop PD motor symptoms
Dysbiosis may amplify neuro-inflammation
This supports the concept that the microbiome may influence disease processes — not just reflect them.
Research published in Nature Communications (Huang et al., 2023) demonstrated microbiome alterations in individuals with REM sleep behaviour disorder — often preceding a Parkinson’s diagnosis.
So let’s look at some early warning signs of Parkinson’s disease
Some lesser-known early signs include:
Reduced sense of smell
A diminished ability to smell common scents such as coffee, food cooking or flowers can occur many years before other symptoms. This may be related to early protein changes in brain areas involved in smell.
Persistent constipation
Slower movement of the digestive tract is very common in Parkinson’s. Changes in the nervous system that regulates the gut, along with alterations in the gut microbiome, may contribute to chronic constipation long before movement symptoms develop.
Changes in handwriting
Handwriting may gradually become smaller, cramped or fade toward the end of sentences. This is known as micrographia and can reflect subtle changes in fine motor control.
Mood changes such as anxiety or depression
Lower dopamine levels can influence brain circuits involved in mood and motivation. Some individuals experience new or unexplained anxiety, low mood or increased worry in the years preceding diagnosis.
Acting out dreams during sleep
A condition called REM sleep behaviour disorder can cause people to shout, punch, kick or physically act out vivid dreams while asleep. This can be one of the strongest early neurological indicators.
Light-headedness when standing
Parkinson’s can affect the autonomic nervous system, which controls blood pressure. Some people experience dizziness or faintness when standing up due to a drop in blood pressure or as it’s called, postural hypotension.
Reduced facial expression
Known as facial masking, the face may appear less expressive, with reduced blinking or smiling. Family members often notice this subtle change first.
A softer or quieter voice
Speech may become softer or more monotone over time due to stiffness and reduced coordination of the muscles used for breathing and speaking.
Subtle stiffness or slowed movement
Early motor changes may include stiffness in one arm or leg, reduced arm swing when walking, smaller steps or a slight shuffling gait.
When to seek medical advice
Many of these symptoms are common and can occur for reasons unrelated to Parkinson’s disease. However, a combination of several persistent symptoms, particularly when they develop gradually over time, should prompt a discussion with a healthcare professional.
Early evaluation can help guide appropriate care, support quality of life and allow earlier access to management strategies.
Why This Matters for my Patients
Parkinson’s disease is increasingly viewed as a potentially preventable systemic inflammatory condition which may be metabolic and immune mediated. Current research is suggestive that neurocognitive function is not simply isolated to the brain and is influenced by whole body health
This is exciting as it this truly opens the door to proactive strategies we can engage to support PD sufferers and aim to slow progression.
Parkinson’s prevention-focused and Functional Care
At the Gut Skin Clinic in Neutral Bay, I engage high level NATA genomic MICROBA microbiome testing to:
assess microbial diversity, numbers and species, not simply in the large intestine but throughout the entire extent of the gut, including the oral cavity. I have previously written on the developing science around oral species population characteristics and neural inflammation / cognitive decline.
evaluate short-chain fatty acid production, your bodies natural anti inflammatory molecules
explore gut barrier function and gut wall integrity
review bowel motility patterns
investigate deeply unhealthy gut bacterial waste products
identify poor representation of the healthiest biome species
Testing does not diagnose Parkinson’s disease.
It provides valuable insight into modifiable terrain and is typically undertaken as part of a multi disciplinary team approach.
Results are interpreted within the context of:
Full clinical history
Nutritional history and habits
Sleep hygiene
Blood markers
Environmental exposure
Metabolic health
Neurological symptoms and their pace of progression
Prevention steps to consider
Comprehensive Microbiome testing
Personalised analysis rather than generic probiotic prescriptions. If working with a practitioner be curious as to their experience with test result interpretation. Microbiome science is relatively new and reports differ, and are very detailed. Understanding nuance and clinical relevance is vital.
2. Address constipation early
Chronic constipation is one of the strongest prodromal associations with PD.
3. Support gut barrier integrity
Optimise fibre diversity, butyrate production, and reduce ultra-processed foods. Be aware that not all fibres suit everyone. I use many differing “functional” fibres in clinic and each is reccomended pursuant to your results. The wrong fibre may exacerbate your gut symptoms.
4. Reduce systemic inflammation
Prioritising Mitochondrial energy production, Glycemic load, Sleep quality and Autophagy combined with regular movement, stress management and review of environmental toxin burden. One of my most rewarding components of my work is supporting clients to understand foods that suit them and are less inflammatory for their unique physiology.
My Key Takeways:
Your gut and brain communicate constantly via immune, metabolic and neural pathways. Your VAGUS nerve, your messenger superhighway.
While the microbiome is not proven to be the single cause of Parkinson’s disease, research supports it as a significant contributing factor.
Proactive gut health optimisation represents low-risk, evidence-aligned strategy for neurological support.
References
Dorsey ER et al. (2018). Global burden of Parkinson’s disease. The Lancet Neurology.
GBD 2016 Neurology Collaborators (2019). Global burden of neurological disorders. The Lancet Neurology.
3. Zachary D. Wallen et al. (2022). Metagenomics of Parkinson’s disease implicates the gut microbiome in multiple disease mechanisms. Nature Communications.
4. Nielsen SD et al. (2021). Gut microbiota and Parkinson’s disease. Brain Research.
5. Ming-Fang Sun & Ying-Qing Shen (2018). Dysbiosis and microbial metabolites in Parkinson’s disease. Ageing Research Reviews.
6. Huang B et al. (2023). Gut microbiome dysbiosis across early Parkinson’s disease. Nature Communications.