How stress hormones block fat loss — even with a perfect diet
I remain committed to guiding and empowering you toward sustained vitality through evidence-based approaches and clear scientific explanations. This topic however consistently ranks among the most challenging for me.
Over decades working in metabolic health and preventive care I hear a very common complaint;
“ Victoria, I’m eating right, exercising and following all the advice — why won’t the weight budge ? ” Patients frustrated by fat that seems impossible to lose, even with a seemingly perfect diet and consistent exercise.
I compassionately believe:
you are not broken
you are not alone
you likely need a realignment metabolically and an emphasis shift, let me explain.
Stubborn weight gain in stressed individuals is common, especially when the HPA axis — the body’s central stress system — is dysregulated or out of balance.
Let’s understand some science behind stress hormones as it can make all the difference.
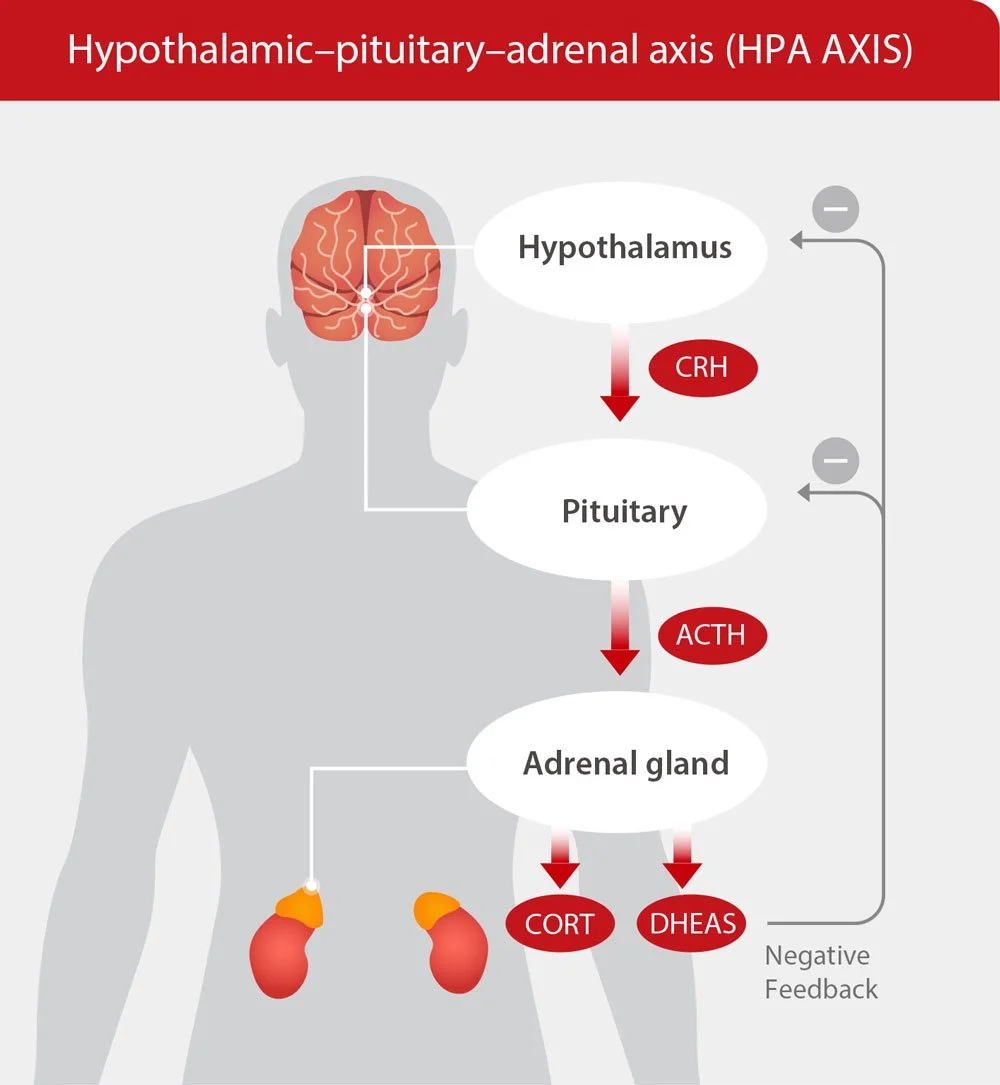
What is the HPA Axis?
The HPA axis connects important parts of your brain, the hypothalamus and pituitary gland with your adrenal glands. This system regulates your body’s stress response.
When you experience stress — emotional, psychological, inflammatory, or even environmental — your HPA axis triggers the release of cortisol, your primary stress hormone.
Cortisol gets a bad wrap but is not all bad and is essential for:
Maintaining healthy blood sugar levels
Supporting brain function and alertness
Modulating immune activity
Calming inflammation
Regulating blood pressure
The problem arises when stress is chronic. Continuous activation of the HPA axis can interfere with your metabolism, quality of sleep, appetite and fat storage — even if your diet is perfect.
Healthy Cortisol rhythm vs chronic stress
In a healthy individual:
Cortisol rises overnight and peaks in the morning to wake you up feeling bright, pain free and ready to embrace the day
Cortisol gradually declines throughout the day
Is lowest at night when you are yawning in the evening to allow for restful sleep (cortisol is related to melatonin with an exquisite inverse relationship)
In chronic stress, Cortisol may be:
Elevated throughout the day
High at night
Blunted in the morning
Standard single morning blood tests often miss these patterns. At Gut Skin Clinic I often review multiple salivary cortisol testings to map the full 24-hour cortisol rhythm. This gives a complete picture and can guide personalised weight loss strategies.
The diagram above explains the continuum of fat storage. Let’s look at some of the mechanisms.
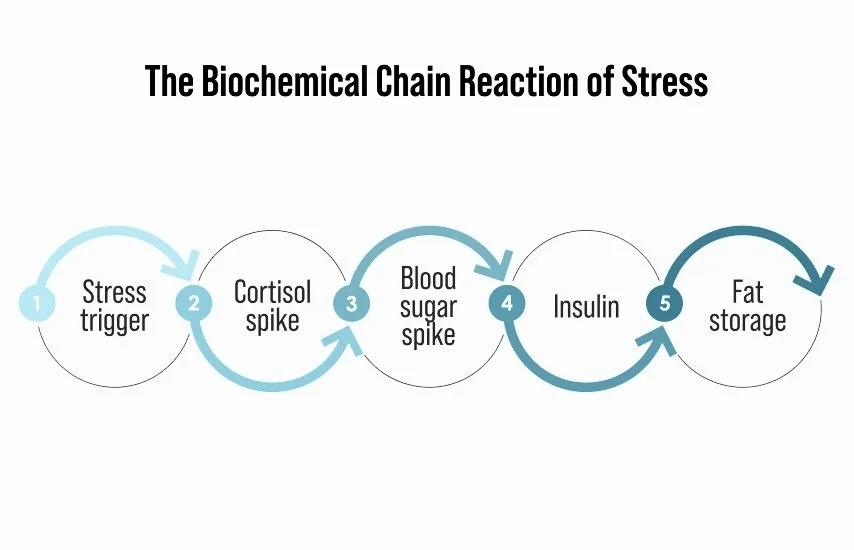
Elevated Cortisol drives fat storage
Cortisol triggers gluconeogenesis in the liver, a process that stores glucose for times of famine or going without, problem is contemporary life is without famine resulting in increased blood glucose even without eating.
Higher blood sugar → higher insulin → fat storage.
Chronic stress leads to:
Insulin resistance
Central fat accumulation
Difficulty losing weight
Even with strict dieting, the body’s hormonal environment favours fat storage over fat burning.
This was me in my early 40s.
Left hand picture, working hard, raising 3 daughters, senior in Intensive care unit and Emergency and teaching at college…. my days featured extreme fatigue, sore joints, skin rashes, gut upsets, moody …. and a subsequent shock diagnosis
Right hand picture 2 years later, well on the way with my healing journey of discovery.
I’m sharing these so your understand that I have not always been of healthy weight. It was at this time I received a significant health scare. Studying Nutrition and understanding that being on the front line in Emergency and Intensive care was making me sick was my FIRST BIG STEP.
I had to change many things, not just to loose over 20% of my body weight but to survive from a life threatening illness. I wanted to enjoy my babies growing up.
My recovery was only possible by understanding, deeply, that the stresses in my life were making me sick. And these stresses took many forms.
This was one of the most powerful times in my life and so changed the whole trajectory of not just my health but who I have become as a practitioner and my wonderful life today.
2. Cortisol increases appetite & cravings
Stress hormones influence hunger signals and cravings. There are multiple studies that demonstrate this in both animal and human models. High cortisol can make you:
Crave energy-dense, high-carb, or salty foods
Eat more than usual, often unconsciously
This is biological, not lack of willpower. Elevated cortisol increases caloric intake and the tendency for emotional eating and fat storage in often the most stubborn places.
3. Cortisol slows metabolism by affecting Thyroid hormones
Cortisol can reduce conversion of T4 to T3 (the active thyroid hormone), slowing metabolism and reducing fat burning.
Lower T3 =
Reduced mitochondrial activity
Lower basal metabolic rate
Less efficient fat metabolism
High cortisol can make cells less responsive to existing T3 and can create symptoms of hypothyroidism even if blood tests appear “normal”.
4. Nighttime cortisol disrupts Sleep & recovery
Elevated evening cortisol impairs sleep, worsens blood sugar control, and further disrupts appetite regulation.
Poor sleep creates a vicious cycle: stress → poor sleep → slower metabolism → more weight gain .
5. Low Cortisol can also be a factor
Some chronically stressed individuals eventually develop blunted morning cortisol, leading to:
Fatigue
Reliance on sugar or caffeine to kick start the day
Anxiety and low motivation
In these patients their weight gain may be driven by inflammation and metabolic dysfunction not simply high or low cortisol alone.
Medically Supervised Weight Loss
At Gut Skin Clinic, I understand that stubborn weight gain is often not your fault. Your body is responding to stress and protecting itself.
My medical weight loss approach focuses on:
Baseline assessment of metabolic health including Body composition analysis, full history, food diary, knowledge of your daily habits and blood results review.
HPA axis clinical assessment and support
Blood sugar stability
Nutritional support personalised to you
Education
Sleep and circadian optimisation
Stress and emotional resilience strategies
in some cases, investigating tissue toxin burden.
Addressing your root causes of hormone and cortisol driven weight gain can give many patients hope by tacking the issue in a different way, not simply to eat less and move more. Patients often see better fat loss outcomes, improved energy, and reduced cravings — even if previous diets and exercise programs failed.
My message to you
If you feel like you’re “doing everything right” but the scale won’t budge, chronic stress and HPA axis dysregulation may be silently sabotaging your efforts.
With personalised assessment and support, you can retrain your stress response and support a healthier metabolism…one good night’s sleep at a time.
References
Epel, E. et al. (2000). Stress and body shape: stress-induced cortisol secretion is consistently greater among women with central fat. Psychosomatic Medicine, 62(5), 623–632.
Rosmond, R. (2005). Role of stress in the pathogenesis of the metabolic syndrome. Psychoneuroendocrinology, 30(1), 1–10.
Adam, T. C., & Epel, E. S. (2007). Stress, eating and the reward system. Physiology & Behavior, 91(4), 449–458.
Tsigos, C., & Chrousos, G. (2002). Hypothalamic–pituitary–adrenal axis, neuroendocrine factors and stress. Journal of Psychosomatic Research, 53(4), 865–871.
Spiegel, K. et al. (1999). Impact of sleep debt on metabolic and endocrine function. The Lancet, 354(9188), 1435–1439.
Heyma P et al (1982) Glucocorticolids decrease in conversion of Thyroxine into 3,5,3- tri-iodothyronine . Journal of Clinical science London. PMID 282948
Microbiome Gut and Regenerative Skin and Hair in Neutral Bay, Cremorne, Mosman, Sydney.
Functional and Nutritional Medicine Practitioner (RN)
Microba Microbiome Practitioner
Skin Health + Hair Restoration
Compounded Skin Nutraceuticals
Professional Food and Nutritional Coach